Understanding Lipedema and Lymphedema Fibrosis
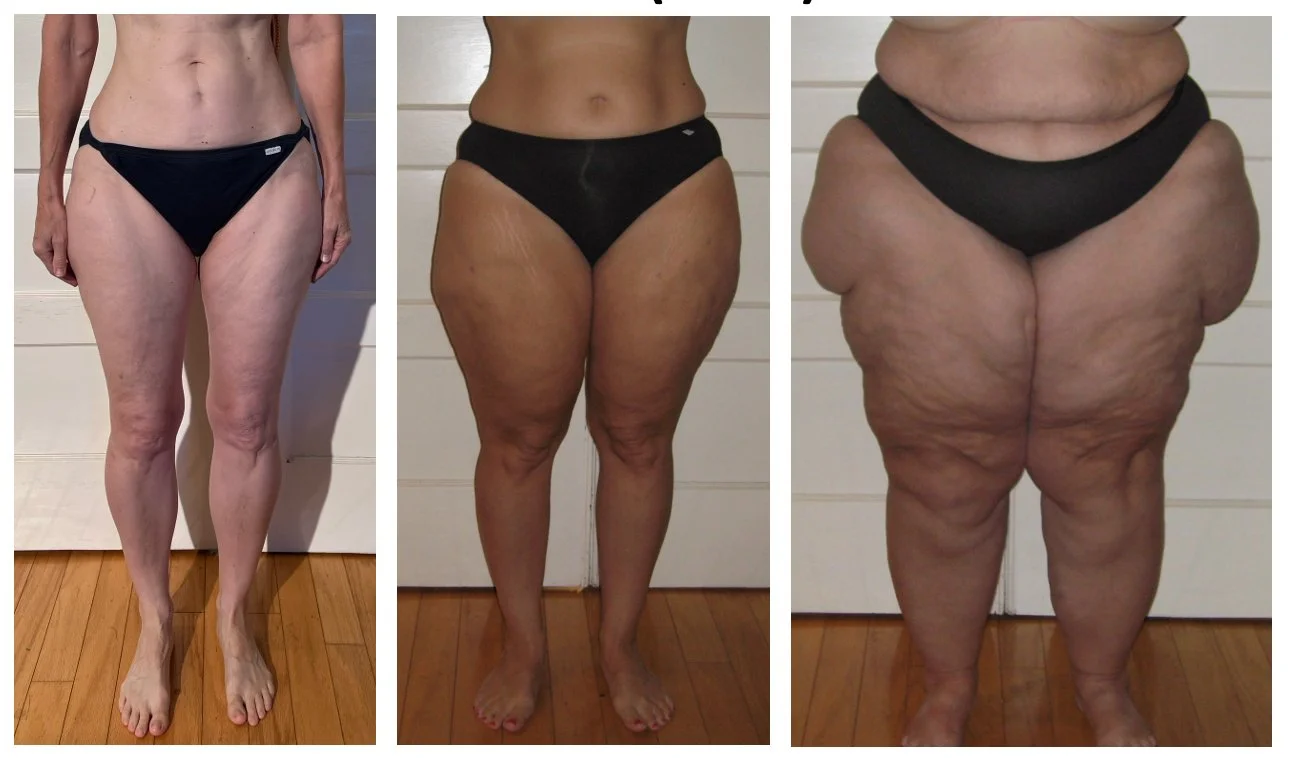
Lipedema, sometimes called “painful fat syndrome,” is a chronic condition primarily affecting women. Lipedema is characterized by a symmetrical, bilateral build-up of fibrotic fat beneath the skin, known as subcutaneous adipose tissue (SAT).
Image credit: © 2025 Karen Ashforth, used with permission
SAT is not like regular fat: it is inflamed and painful, and can grow progressively harder and larger. It is common to have hard and painful nodules within the lipedema SAT ranging in size from rice-like, to walnut sized, or even larger.
Lipedema is often seen in the lower half of the body, creating a disproportionate appearance. The feet are rarely affected in the early stages but can develop symptoms over time. Lipedema can also be present in the lower torso and in the arms.
Onset of lipedema appears to be linked to periods of hormonal change such as puberty, pregnancy and menopause. In these transitions, women can feel particularly vulnerable about body image, and dealing with lipedema can affect emotional well-being.
Some of my lipedema patients tell me that they have trouble going outside their home because they feel so self-conscious. As a therapist, I feel it is important to not only provide education and treatment to empower my patients to manage their symptoms, but to also give emotional support and encouragement. I often recommend the many online resources for lipedema, which provide a wide array of education and support.
Although lipedema is related to lymphedema and many treatments are similar, it is critical for patients and professionals to understand the unique aspects of lipedema. The name “lipedema” literally means swelling in fat. It is important to address this inflammation found in lipedema.
How is Lipedema Different from Obesity?
Lipedema is not the same as obesity, although it is possible to have both. Unlike obesity fat, lipedema SAT is painful and inflamed. Lipedema SAT can be limited to a few places, giving the body a disproportionate appearance. Obesity is characterized by widespread fat over the entire body, with two major patterns of fat distribution: gynoid (pear shape) and android (apple shape). Because a common presentation of lipedema is in the lower body, lipedema can be confused with, and mis-labeled, as gynoid obesity.
When the two are present together, obesity can worsen lipedema and should be addressed. Although calorie restriction can yield weight loss with obesity, it does not impact SAT. This can be discouraging, because women with lipedema can use calorie restriction to lose weight and fat mass from some parts of the body, but there is minimal reduction in other parts. Having said that, there are dietary programs that have recently emerged that are helping lipedema.
Lipedema and Lymphedema: Similarities and Differences
Lymphedema occurs when there is some type of failure to the lymphatic system. In primary lymphedema the lymphatic system is congenitally malformed. In secondary lymphedema, the previously normal lymphatic system has become injured due to disease, surgery or trauma. The concept of “Lipo-Lymphedema” is currently being questioned because it is recognized that lymphedema can be present in any stage of lipedema.
The chronic inflammation present in lipedema causes fibrotic damage: SAT and nodules grow larger and becomes harder. If the lymphatic vessels are damaged by inflammation and fibrosis, lymphedema can accumulate and worsen.
Although lipedema is often confused with lymphedema and obesity, lipedema has unique characteristics that set it apart. It can be further confusing when lipedema is present with obesity and/or lymphedema. I’ve summarized some of the major characteristics in these lists, to show differences between lipedema, lymphedema and obesity:
Lymphedema:
Gender: males and females
Onset: any age
Hereditary: primary lymphedema is hereditary, secondary lymphedema is not
Areas affected: any part of the body including the head, torso, abdomen, often asymmetrical
Body Mass Index (BMI): can be normal
Pitting: present at any stage but mostly early stages
Hand and feet: swelling can be present at any stage
Kaposi-Stemmer’s sign: positive
Painful: yes, in some patients
Bruising: requires significant trauma
Obesity:
Gender: males and females
Onset: any age
Hereditary: in some cases
Areas affected: usually entire body, may have gynoid (pear) or android (apple) fat distribution
Hands and Feet: affected
BMI: elevated >30
Fat distribution: both superficial (under skin) and deep (around organs)
Diet: responds to calorie restriction, fat and weight loss generally occur throughout body
Kaposi-Stemmer’s sign: negative
Painful: no
Bruising: requires significant trauma
Can aggravate lipedema and lymphedema symptoms
Lipedema:
Gender: almost exclusively females
Onset: mainly at times of hormonal fluctuation: puberty, around childbirth or menopause
Hereditary: often affects other female family members
Areas affected: always bilateral (both sides), primarily lower body, upper body 30% time
BMI: can be normal
Fat distribution: increased fat under skin: subcutaneous adipose tissue (SAT)
Hands and feet: usually not affected in early stages
Kaposi-Stemmer’s sign: negative in early stages
Diet: not responsive to traditional diet and exercise: with calorie restriction, weight loss usually occurs in areas not affected by lipedema
Painful: yes, in almost all patients
Bruising: easily bruised due to increased capillary fragility
Hypothermia of skin
Image credit: © 2025 Karen Ashforth, used with permission
What are the Different Types of Lipedema?
Lipedema has five distinct patterns of increased SAT distribution in the body:
Type I: Pelvis, buttocks and hips
Type II: From buttocks, to knees, folds of fat on the inner knees
Type III: From buttocks to ankles, “cuff” of tissue overhanging ankles
Type IV: Arms and sometimes hands
Type V: Legs/Knees to ankles, “cuff” of tissue overhanging ankles
What are the Stages of Lipedema?
Lipedema is a progressive condition that can become more serious if it is not treated. Because lipedema responds well to treatment in stage 1, the earlier it is addressed, the better.
Stage 1:
Skin surface is normal
SAT soft
Nodules may be present ranging in size from rice-like to walnut-shaped
May have swelling
Responds well to treatment
Stage 2:
Skin surface becomes uneven and harder with “mattress pattern” indentations
SAT hardens, indentations visible, larger
Nodules increase in size, become harder, can become stuck together
May have swelling
May respond well to treatment
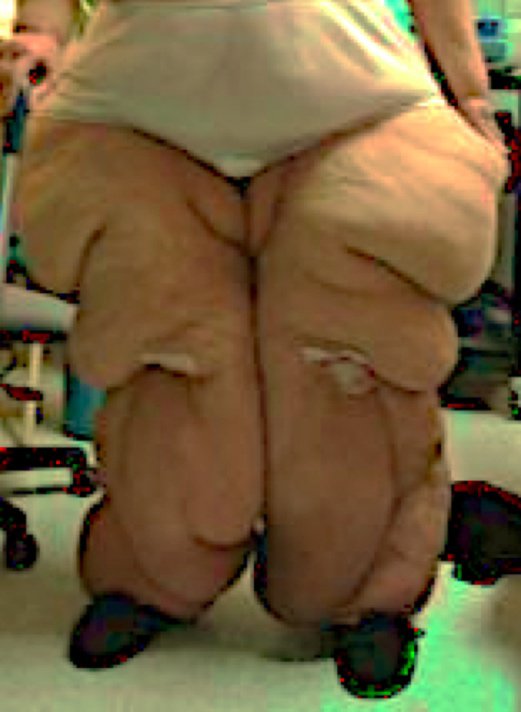
Stage 3:
Skin surface thick and hard, peau d’orange, (orange peel-like quality),
SAT increases and continues to harden
Nodules are large
Fat pads and lobules (large masses of tissue that overhang) especially on thighs, knees, and ankles
May have swelling
Less responsive to treatment
Stage 4:
Some literature has identified a fourth stage as Lipo-Lymphedema (lipedema with lymphedema), but this is currently being questioned because lymphedema can be present in any stage of lipedema.
Lipedema Treatment:
Complete decongestive therapy (CDT): is used to treat both lymphedema and lipedema. CDT consists of manual lymphatic drainage (MLD), exercise, compression bandaging, compression garments, and skin care. CDT helps lipedema by decongesting swelling, encouraging normal lymphatic vessel pumping, and decreasing pain.
Manual lymphatic drainage (MLD): MLD is a gentle massage that directs lymph fluid out of swollen areas and assists the body’s lymphatic drainage patterns. It is performed by a certified lymphedema therapist, who can also teach people with lipedema to perform it on themselves. MLD can be very relaxing, can decrease pain, and stimulate lymphatic circulation. MLD is known to decrease capillary fragility in lipedema. Applying compression garments after MLD help keep the reduction effects.
Compression bandaging and garments:
Compression garments help to compensate for loss of skin elasticity and provide support to tissues. This can decrease pain and enhance muscle pumping action to move fluid out of swollen areas. Compression provides containment to maintain the reduction of swelling after MLD, and prevent fluid from reaccumulating. This helps the body feel less heavy and can make it easier to move and walk. Ultimately, wearing compression garments helps prevent lipedema pain and help the lymphatic and vascular circulation.
In order to maximize comfort in garments, it is important to strike a therapeutic balance between the amount of SAT, severity of swelling, and degree of compression. Medical grade (>20-30 mmHg) compression garments may be painful to wear and difficult to put on and take off.
Textured circular knit compression garments have less compression (12-21 mmHg) but the micro-massage created by the weave in the fabric stimulates the superficial lymphatics, and compensates for having less pressure. They are also generally more comfortable to wear and easier to put on and take off, but may not be strong enough to support larger bodies. In those cases, custom elastic flat knit or Velcro wraps might be better compression alternatives.
Types of compression can be layered, or different garments can cover different parts of the body depending upon need. For instance, it is possible to achieve a compression gradient and comfort using a textured elastic capri garment to compress the hips, thighs, and knees with lower legs compressed by Velcro wraps or custom flat knit elastic compression stockings. Quilted compression can also be effective, but it is bulkier and hotter to wear.
A caution: if compression is only used on swollen areas that are closer to the trunk such as thighs and knees, the uncompressed lower legs and feet are vulnerable to increased swelling, much like squeezing the middle of the toothpaste tube.
Exercise: This is very important because the vascular and lymphatic systems rely on the pumping action of muscles to move fluid. Deep breathing and muscle contraction increase oxygen in the body’s tissues, and hypoxia (low oxygen) is thought to be an important factor in lipedema. Deep water exercise is particularly beneficial for those with lipedema. Hydrostatic pressure and buoyancy can enhance the muscle pumping action, help prevent injury, and decrease weight on the joints during exercise. However, over exercising is harmful to SAT tissues by building up lactic acid and oxidants.
Skin Care: It is important to keep the skin moisturized and healthy: this creates a good barrier to prevent infection.
Elevation: Elevating legs periodically during the daytime helps harness the effects of gravity to help with orthostatic swelling that occurs in stage 1 lymphedema. It can also be helpful when combined with more aggressive treatment.
Pneumatic compression: If conservative treatment of elevation, compression, and exercise do not yield significant changes in swelling, pneumatic compression can be helpful. During pneumatic compression, patients put on an appliance that contains individual air chambers and the chambers inflate sequentially from the hands or the feet towards the trunk.
There is much research to support the benefits of pneumatic compression for lipedema and lymphedema. Evidence points not only to pneumatic compression stimulating lymphatic circulation and reducing swelling, but also to pain reduction and decreased capillary fragility in lipedema.
An additional benefit is that pneumatic compression promotes relaxation.
Many insurances pay for this equipment for home treatment; however, Medicare will not cover pneumatic compression with only a lipedema diagnosis, however, a lymphedema diagnosis is covered.
There are a number of options for pneumatic systems, including those which accommodate larger sized people. The ability to adjust the pressure and programming to find both comfort and effective treatment is important.
Nutrition:
Lipedema SAT is not responsive to calorie reduction, and in the past, lipedema was believed to not be affected by diet at all. In the last few years, two groups of experts in lipedema have emerged with guidelines that are proving effective in helping lipedema.
Image credit: © 2025 Karen Ashforth, used with permission
Both groups acknowledge the unique characteristics of lipedema fat, and how it differs metabolically from “regular” fat. Regulating insulin production and normalizing estrogen levels appear to have marked effects on both regular and lipedema fat. These books represent two approaches that offer dietary choices to lower inflammatory, hormonal and metabolic factors in lipedema and lymphedema.
Lymphedema and Lipedema Nutrition Guide (Ehrlich et al, 2016) is authored by physicians and clinicians specialized in lipedema and lymphedema treatment. It includes specific guidelines about recommended eating patterns that “starve” lymphedema and lipedema. Emphasis is on eating whole foods, limiting animal protein, and avoiding refined grains, added sugars, most dairy products, and chemically modified fats. Specific nutritional supplements are recommended.
The Ketogenic Solution for Lymphatic Disorders (Keith 2019) is written by an occupational therapist and certified lymphedema therapist who earned her doctorate studying the effects of the ketogenic diet with lymphedema and lipedema patients. The ketogenic diet has been in use for over a century and is supported by a wide body of research. Guidelines emphasize specific proportions of healthy fats, proteins, and limited low glycemic (low sugar/starch) carbohydrates.
There are numerous recent research studies to prove the ketogenic diet helps specifically helps women with lipedema lose fat and inches from the areas of their bodies affected by lipedema, sometimes for the first time in their lives.
Why Introduce Antifibrotic Treatment Gradually?
As with lymphedema, fibrosis is present in all stages of lipedema, but the types of fibrosis are unique to lipedema. Therefore, special approaches and techniques are necessary to address lipedema fibrosis. Lipedema fibrosis can be further complicated by other types of fibrosis such as surgical scar tissue, radiation-induced fibrosis, post-cellulitis fibrosis, or lipodermatosclerosis. Specific treatment for those types of fibrosis have been discussed in my previous articles; you can find them on my website: https://www.karenashforth.com
One of the biggest caveats of antifibrotic treatment is to work within pain tolerance and not try to be too aggressive right away. The deeper and more aggressive treatments used for lymphedema-related fibrosis can be more painful, and create more bruising when used with lipedema-related fibrosis. If approached gently, many lipedema patients are willing to trade the temporary pain and mild bruising side effects in exchange for softer, lighter tissues, as well as increased function and mobility.
Fibrosis treatment will be more successful if any swelling is addressed first. After performing decongestion, anti-fibrotic techniques can be introduced gradually, in small doses. Educating the lipedema patient about types of treatments, and the benefits of each can build trust, and encourage participation.
These techniques are highly specialized and not taught in basic lymphedema training programs. It is important that practitioners be experienced in lymphedema and lipedema treatment, and also be properly trained in advanced techniques before incorporating them into treatment.
How is SAT different from lymphostatic fibrosis?
Lymphostatic fibrosis is a fatty matrix created by the inflammatory process in chronic swelling. Lymphostatic fibrosis begins as a high protein swelling that gradually attracts fat cells, which promotes adipogenesis, and creates of fatty tissue.
SAT is also created by an inflammatory process, but the fat is softer and fluffier than lymphostatic fibrosis. The easy bruising in lipedema is a result of the fragility of capillaries in the SAT.
What are SAT Nodules?
Fibrosis forms around the subcutaneous fat cells, creating nodules. These can range in size from a grain of rice to the size of walnuts, or even larger. If lipedema progresses, nodules can adhere to each other and the SAT, creating large, lumpy, painful masses. In later stages of lipedema, large pendulous lobules of SAT can form, which can make it challenging to find well-fitting clothing, and may interfere with sitting, standing or walking.
Specific Anti-Fibrotic Treatments:
Having a large toolbox of techniques allows practitioners versatility in treatment. Some techniques are gentle and others are very aggressive. After swelling is addressed with CDT, these techniques literally go deeper, and can provide significant results. As with lymphedema-related fibrosis, “tune-ups” may be needed. Depending upon the individual and the technique, it may be appropriate to incorporate some fibrosis treatments into the home program.
Manual therapy: There are anti-fibrotic manual therapy techniques for lymphostatic fibrosis that can be helpful for lipedema fibrosis. Some CDT training programs teach deeper manual techniques. Other deep tissue massage techniques, such as myofascial release, or the Chinese massage technique of Tui Na, can be helpful in treating fibrotic SAT and nodules.
Of interest is a manual technique specifically directed towards SAT, available mainly in the Netherlands. It is a full body treatment that softens SAT. Treatment begins superficially, then pressure deepens over subsequent treatments to address muscle and fascia layers all the way to the bone.
Dr. Karen Herbst studied this technique over a four-week period in 2017, with a group of seven women with lipedema and Dercum’s disease. Effects of the treatment were significant, and included decreases in fibrosis, pain, leg volume and body fat. Some participants also experienced improved SAT structure. Treatment side effects found during the study were pain, bruising and heartburn.
Despite that, all participants said they would recommend this treatment to women with lipedema. Although the pilot study was small, it demonstrated that aggressive techniques were effective in helping lipedema-related fibrosis. A seminar for certified lymphedema therapists was offered in the same time period as the study, and opened the door for lymphedema practitioners to successfully incorporate more aggressive anti-fibrotic techniques into lipedema treatment.
Compression: There are many types of compression garments and pads that have anti-fibrotic effects. Textured elastic compression garments (either non-medical grade or custom flat knit) can provide a gentle anti-fibrotic effect to hardened skin, SAT, and nodules. Bulkier quilted compression with more irregularly textured filling, such as chipped foam, foam strips, or cherry pits, can be useful. These pads and garments can be gentle or aggressive depending upon the medium and the amount of pressure used over them.
It should be noted that cherry PitPaks must be used cautiously with sensitive skin, or altered sensation. For patients with high levels of pain, PitPaks are best used for a brief trial of 30-60 minutes with a skin inspection and pain assessment before using for longer periods. PitPaks or chip foam quilted compression pads may be placed inside of other compression garments to address hardened areas of tissue. Quilted garments cover a much wider area than pads, but are bulky and may be best suited to wearing at night or during pneumatic compression treatment.
Low level laser: The anti-inflammatory and anti-fibrotic effects of near infra-red (non-thermal) light therapy are useful prior to and along with manual or instrument techniques. The aperture of the laser can even be used as an anti-fibrotic instrument while delivering light therapy.
TENS (transcutaneous electrical stimulation): This modality has been used medically for decades to lower pain and inflammation. On certain settings (extremely low frequency), it can stimulate the body to produce endorphins, which help to control pain. TENS was shown to help reduce pain, reduce SAT, and increase function in a single study of a man with Dercum’s disease. Because of the anti-inflammatory effects of TENS, it may be a potentially useful treatment for rare adipose disorders.
Vibration: This has been shown to stimulate vascular and lymphatic circulation, reduce pain, and reduce inflammation in people with lymphedema. It can also be useful for those with lipedema, and with proper training, can be a good addition to the home program. Hand held vibrators have historically been used clinically to remodel many different types of hardened scar tissue. Whole body vibration has been found to be an effective treatment for lymphedema and lipedema.
Elastic taping: This is used widely in many medical settings, including treatment for lymphedema, sports injuries and neurological conditions. Benefits include pain management, edema management, scar tissue remodeling, posture management, and neuromuscular facilitation. A specialized, highly adherent tape “lifts” skin to improve superficial circulation.
The mechanical pull of the tape creates gliding of adhered tissues to soften fibrosis. It is very important to determine skin tolerance prior to treatment to avoid irritation. Tape must be removed properly to avoid tearing skin. Taping can cover large areas of SAT fibrosis, and is useful for providing support, and decongesting fat pads and lobules. There are many applications, techniques, caveats and contraindications which make special training essential. It is particularly important to try a test strip on a very small area first to make sure that it can be tolerated on a larger area.
Instrument assisted soft tissue mobilization: This technique is based on the Chinese “Gua Sha” treatment which traditionally uses ceramic or jade instruments to provide a deep massage to tissues. It is also known as Graston Technique, Sound Assisted Soft Tissue Mobilization or Astym. There are now many different variations of the basic technique, with tools ranging from surgical steel to plastic.
This treatment creates a controlled microtrauma that remodels tissues. Techniques can range from very gentle to very aggressive. Side effects can include pain, bruising, and petechiae (broken blood vessels). When instrument massage is performed for people without lipedema, these side effects usually resolve within 48 hours, but they can last much longer if performed on lipedema fibrosis due to fragile vasculature. Because of this, it is critical to have proper training in these techniques, as well as to use caution, and monitor side effects.
Negative pressure: This is based on traditional Chinese medicine “cupping.” This technique relies on a gentle suction that lifts and separates layers of tissue that are stuck together. Like instrument massage, this technique can create a controlled microtrauma to remodel tissues, and has similar potential side effects of pain, bruising, and petechiae. Some specialized negative pressure equipment can offer a variety of calibrated and controlled pressures as well as adjunctive treatments such as vibration. Negative pressure should never be attempted without training, and should not be used aggressively with lipedema.
Hivamat: This is an oscillating electrical modality used in lymphedema treatment, and has been studied as a decongestive agent for lipedema. It is gaining popularity clinically for treatment of many different types of lymphedema and lipedema-related fibrosis.
Pneumatic compression: While most people think of pneumatic compression as a decongestive treatment, it can also be a powerful anti-fibrotic agent. Using chip foam pads or garments during a pneumatic compression treatment can create a gentle effect that can soften tissues progressively as treatment is repeated over time. Some patients are able to tolerate PitPaks under pneumatic compression, but this treatment is very aggressive. It is advised to determine tolerance first, before using PitPaks with pneumatic compression.
Using higher pressures can create a deeper and more powerful treatment. Higher pressures may be required to give a therapeutic treatment in the later stages of lipedema if tissues are hard and bulky, or if obesity is also present. Pressure should always be adjusted to tolerance.
Most pneumatic compression devices have the capability for one or both types of commonly used compression programming: sequential and peristaltic. Both programs start the cycle of inflation at the hands or feet and chambers are inflated, moving in the direction of the torso. With sequential programs, each chamber stays inflated until all chambers are inflated, and then all deflate at the same time before starting a new cycle. In peristaltic programs, only 1-2 chambers are inflated at a time, forming a wave-like action.
Peristaltic programming can be more comfortable for women who have pain issues with compression, especially if higher pressure is required to move fluid through bulky tissues and remodel fibrosis. As fibrosis softens and tissue volume decreases, less pressure may be needed. It is important to make sure that pressure is always regulated to a comfortable level.
Sequential programs provide a more aggressive treatment for fibrosis, but overall pressure may need to be lowered if hands or feet are uncomfortable from the sustained pressure held through the entire cycle. A way to minimize this problem is to select a pneumatic compression device that has a rapid cycle time and longer pause time, to avoid prolonged pressure on hands and feet.
There are a number of different appliances used with pneumatic compression.
Type I, II, III lipedema: A pantsuit appliance that treats both legs, groin, hips, buttocks, and abdomen is most appropriate. Some appliances that treat legs and abdomen have a gap in the crotch, leaving the genitals and lower buttocks without treatment, and increasing the risk for developing more swelling and fibrosis in these areas. Larger appliances are available for those with later stages of lipedema, or a combination of lipedema and obesity. These must be used with specialized pumps that are capable of inflating larger appliances.
Type IV lipedema: Swelling in the arms/hands can be addressed by single arm sleeves. Lipedema can sometimes be present in the mid-back or lower ribcage area of the torso, in which case a jacket appliance that treats the torso is best.
Type V lipedema: If swelling is only present in the lower legs, leg sleeve appliances are appropriate, but if swelling progresses to the upper thighs, a pantsuit appliance is the best choice.
The success of the treatment is directly affected by how well the appliance fastens and conforms to the body. Some pumps have sensors that work with zipper-closure appliances that give feedback during inflation to deliver the specified dosage of compression while inflating to fit, conforming evenly around the body.
Velcro-closure appliances rely on the ability of the user to close the Velcro correctly each time to conform to body contours and must be adjusted if body size changes. The entire appliance must be closed correctly to prevent areas of irregular pressure, which could leave some areas untreated. Additionally, if fastened loosely, the treatment will not deliver the specified pressure.
With either type of closure, patients with large lobules or large variation in diameter within a limb may need to use padding, as is done with compression bandaging. Towels or small pillows make effective padding to ensure even compression with irregularly shaped limbs.
Therapy balls: Soft and hard balls come in small and large sizes, and can even have surface texture. They can be used to treat fibrosis by using the weight of the body to “melt” tissues against the ball. Pressure is controlled by body posture. The most control and least amount of pressure is achieved while standing with the ball between the body and a wall. There is extreme pressure when lying on the ball either face up or face down. Pressure can be static or dynamic: the body can rest against the ball or move back and forth to create a massaging effect. Hard balls should not be used for more than 60 seconds due to potential bruising.
Foam rollers: Foam rolls are available in different sizes and textures. They can cover a large surface area, and also be used in numerous positions to create a self-massage to fibrotic areas. Foam rolls made from hard closed-cell foam may create more discomfort than soft balls, and should be approached cautiously.
Ultrasound cavitation: there is emerging interest in the use of Extracorporeal Shock Wave Therapy (ESWT) and US cavitation, which is often combined with negative pressure and light therapy. Evidence is still sparse but they both show promise for helping treat lipedema SAT.
Surgery: Liposuction has become increasingly popular as a means of removing lipedema SAT and is now covered by some insurances in the US. Lymph sparing liposuction techniques, such as tumescent liposuction or water jet assisted liposuction, are preferred for lipedema and lymphedema over traditional liposuction and debulking surgeries. These specialized techniques are more efficient at removing SAT, have fewer side effects, and are less likely to damage lymphatic vessels.
Longitudinal studies post-surgery have demonstrated sustained improvements in size, swelling, pain, heaviness, function and quality of life. However, liposuction cannot completely remove all lipedema SAT and it is possible that remaining tissue can grow over time and, in some cases, even return to prior symptoms. It is also possible to develop lymphedema as a side effect of liposuction. It should be noted that those with Dercum’s disease who have SAT excision have a 50% likelihood of recurrence of SAT.
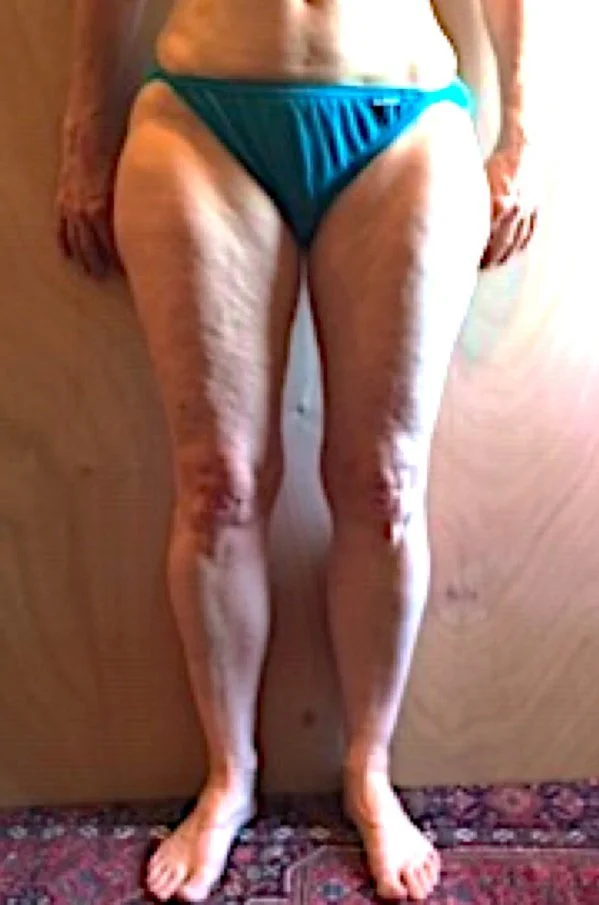
The Impact of Fibrosis Treatment on Lipedema:
Going beyond basic lipedema and lymphedema treatment can be invaluable for individuals with lipedema. Anti-fibrotic treatment to remodel SAT and lobular fibrosis can impact lymphatic and vascular circulation, pain, mobility, body size, and may help prevent the progression of lipedema. Providing empowerment with education, clinic treatment, and an effective home program can create hope and a higher quality of life.
About the Author: Karen Ashforth, MS, OTR/L, CLT-LANA has practiced as an occupational therapist for over 40 years. Specializing as a board-certified hand therapist led to her interest in lymphedema and fibrosis over 20 years ago. Karen’s passions in lymphedema and lipedema practice are equipment innovation and development, treatment of underlying fibrosis and inflammation, and assessment of complex and difficult cases.
She currently works at St. Joseph’s Medical Center in Stockton, California, is an adjunct faculty member with the University of the Pacific in the Doctoral Physical Therapy Program and has a private virtual consulting practice at www.karenashforth.com.
Karen speaks frequently about lymphedema and lipedema at academic, clinical and professional settings and performs clinical research that she presents and publishes nationally and internationally.